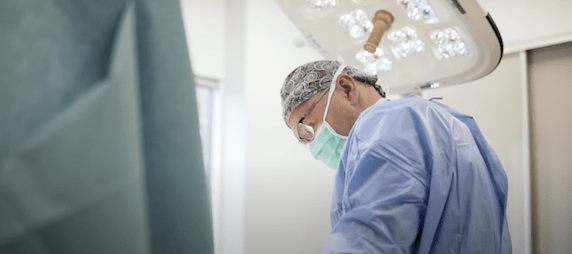
Knee Replacement Abroad: in Lithuania
We are one of the leading orthopaedic surgery clinics for medical tourists in the European Union. We are proud of the fact that over 90 % of our patients come from the UK, Ireland, Norway, Sweden, the United States, Canada and other countries.
Reviews & Facebook group
Our patients and clinic in the media
Prices
- knee replacement surgery package – approx. from 7.040 £
- surgery – 3.470 £
- high quality knee implant – from 2.870 £
- 7 days of uniquely designed outpatient rehabilitation (21% better results*) – 700 £
- joint injection (beneficial for bilateral joint pain) – from 33 £
- long standing x-rays (exclusive, performed in 1 day) – FREE
- 2 online prehab consultations (upon request) – 86 £
Free choice of newest generation implants: Zimmer Biomet, Smith & Nephew and other.
- high tibial osteotomy – from 4.130 £
- knee arthroscopy – from 750 £
- accommodation with medical care – from 62 £ per night
*Comparing to our other option of inpatient rehabilitation. Results are based on the patient survey conducted using internationally acknowledged HOOS/KOOS questionnaires. Read more
- consultation with the surgeon
- necessary health tests
- surgery
- implants
- anaesthesia
- hospitalisation
- 24/7 personal assistance during your stay
- transfers to / from the airport, hotel and clinic
- all documents translated in English
The clinic uses Zimmer Biomet, Smith & Nephew and other highest quality implants. The implant option is discussed in detail once the surgeon reviews your individual case.
Get your surgery for free by claiming a refund from your local health board. The clinic helps patients with the documents needed to claim a refund after following the EU directive route for medical treatment abroad. It applies to patients who are insured under the systems of one of the EU countries and may not get the surgery due to long waiting times.
- knee replacement surgery package – approx. 8.440 €
- surgery – 4.160 €
- high quality knee implant – from 3.440 €
- 7 days of uniquely designed outpatient rehabilitation (21% better results*) – 840 €
- joint injection (beneficial for bilateral joint pain) – from 40 €
- long standing x-rays (exclusive, performed in 1 day) – FREE
- 2 online prehab consultations (upon request) – 100 €
Free choice of newest generation implants: Zimmer Biomet, Smith & Nephew and other.
- high tibial osteotomy – from 4.660 €
- knee arthroscopy – from 900 €
- accommodation with medical care – from 74 € per night
*Comparing to our other option of inpatient rehabilitation. Results are based on the patient survey conducted using internationally acknowledged HOOS/KOOS questionnaires. Read more
- consultation with the surgeon
- necessary health tests
- surgery
- implants
- anaesthesia
- hospitalisation
- 24/7 personal assistance during your stay
- transfers to / from the airport, hotel and clinic
- all documents translated in English
The clinic uses Zimmer Biomet, Smith & Nephew and other highest quality implants. The implant option is discussed in detail once the surgeon reviews your individual case.
Get your surgery for free by claiming a refund from your local health board. The clinic helps patients with the documents needed to claim a refund after following the EU directive route for medical treatment abroad. It applies to patients who are insured under the systems of one of the EU countries and may not get the surgery due to long waiting times.
Knee replacement case analysis
Patient stories
Only we can offer:
One of the most experienced orthopaedic surgeons in Europe. More than 5.000 joint replacement surgeries were performed by our surgeon to this date.
More than 150 scientific articles co-authored by our surgeon and over 50 publications in different medical journals.
More than 370 positive reviews from our happy clients from all over the world.
Patients saved this number of years by travelling to our clinic instead of waiting for surgery at home country.
Clinic videos
Nordorthopaedics Center Of Excellence

Experienced hip and knee surgeon

- More than 20+ years of working experience
- Over 5.000 joint replacement surgeries performed
- Co-author of 150+ scientific articles
- Read more
Refund for EU patients
Get your surgery for free by claiming a refund from your local health board. The clinic helps patients with the documents needed to claim a refund after following the EU directive route for medical treatment abroad. It applies to patients who are insured under the systems of one of the EU countries and may not get the surgery due to long waiting times. On average our patients from the EU countries get fully refunded by their local health board in 5 months after their surgeries.
Rehabilitation packages
One of the most important factors for a quick and full recovery after surgery is proper rehabilitation. Rehabilitation helps recover after surgery as well as prevents formation of blood clots and helps avoid most of the postoperative complications and side effects. We offer two different rehabilitation packages:
Outpatient rehabilitation results in 21% higher quality of life after knee replacement surgery as compared to our other option of inpatient rehabilitation. The results are based on the patient survey conducted using internationally acknowledged HOOS/KOOS questionnaires.
Outpatient rehabilitation in Kaunas with a physiotherapist. The rehabilitation clinic is equipped with modern facilities. Individual rehabilitation programs are prepared by a kinesiologist with over 20 years of experience, Prof. Laimonas Siupsinskas. This type of rehabilitation is best suited for people who are physically active, athletes and those wishing to return to sports as soon as possible.
Rehabilitation in Kaunas – € 120 / £ 100 for one 1 h physiotherapy session per day.
- personalized rehabilitation course;
- specialist who is also a physiotherapist for Lithuanian Men’s National Basketball Team;
- all required medication;
- transportation to/from the rehabilitation clinic;
- read more about outpatient rehabilitation in Kaunas.
Inpatient rehabilitation at SPA resort in Druskininkai. It is equipped with modern facilities. The professionals there have years of experience working with people after various surgeries and injuries.
Rehabilitation at SPA resort in Druskininkai – from € 220 / £ 183 per day
- personalized rehabilitation course;
- room with TV and private bathroom;
- three meals a day;
- all medication needed;
- transportation to/from the rehabilitation centre;
- read more about inpatient rehabilitation in Druskininkai.
Our clinic
Self-catered accommodation with medical care
11 reasons that make us the most popular orthopaedic clinic abroad
One of the most important factors for a quick and full recovery after surgery is proper rehabilitation. Usually, clinics are not able to offer this due to costs savings. Our patients can choose between two inpatient and outpatient options: rehabilitation with a physiotherapist of the Lithuanian national basketball team, prof. L. Siupsinskas or rehabilitation at a medical SPA.
Our team of 5 orthopaedic surgeons has 10-20 years of experience in the field in total performing over 1.000 different orthopaedic surgeries per year. Moreover, our surgeons are members of various prestigious surgical societies both Lithuanian and international. Our leading joint replacement surgeon S. Tarasevicius is an author of 150 scientific publications in different medical journals, who has performed more than 3.500 joint replacement surgeries during 15+ years of his professional experience.
We are one of the leading orthopaedic surgery clinics for medical tourists in the European Union. We are proud of the fact that over 90 % of our patients come from the UK, Ireland, Norway, Sweden, the United States, Canada and other countries.
One of the world’s leading medical technology companies and orthopaedic implant manufacturers, Smith & Nephew, have chosen Nordorthopaedics as Center of Excellence in the Baltic States.
We are trusted by our patients and we appreciate all the reviews and feedback collected over the years. Find more than 150 testimonials here or on Google.
Already more than 4.000 of our former, current and future patients joined our online community with the aim to build a space for opinions and mutual support. Members are welcome to share experiences about their visit to the clinic and to discuss all surgery-related matters. No other orthopaedic clinic can offer such group support.
Being a true member of the International Society of Arthroplasty Registries, Lithuania is one of the leaders in low joint replacement revision rates, as only 9% of surgeries in Lithuania require revision in 10 years after surgery. Moreover, with the implants used at our clinic, only 2-3% of surgeries require revision in 10 years after surgery, while revision rates in some other Western countries, for example, USA, is as high as 17% in 10 years after surgery. The implants used at our clinic have been evaluated by other countries’ registries as those ensuring longest implant life, as compared to products of other manufacturers. Moreover, thanks to our active participation in collecting data for the registries, the surgical technique used at our clinic ensures best surgical outcomes.
Our clinic is seen on different media mentions like: BBC News, BBC Radio, The Telegraph, MailOnline, Winnipeg Free Press, CTV News, CBC, RTE Radio, itv.
Our clinic works according to the highest standards set by the European Union. This helps to guarantee the quality of medical services. We care about the safety, comfort and successful results of our patients from all over the world.
The clinic helps patients with the documents needed to claim a refund after following the EU directive route for medical treatment abroad. It applies to patients who are insured under the systems of one of the EU countries and may not get the surgery due to long waiting times.
We provide customer service in 9 foreign languages including English, Swedish, Norwegian, Danish, Italian, Spanish, French, Russian, Polish. Everyone in our clinic speaks English, including nurses, assistants and the surgeon.
Athletes treated at Nordorthopaedics
Official clinic of Lithuania national football teams

Highest quality implants
Our clinic uses implants based on their performance in international registries.
Being a true member of the International Society of Arthroplasty Registries, Lithuania is one of the leaders in low joint replacement revision rates, as only 9% of surgeries in Lithuania require revision in 10 years after surgery. Moreover, with the implants used at our clinic, only 2-3% of surgeries require revision in 10 years after surgery, while revision rates in some other Western countries, for example, USA, is as high as 17% in 10 years after surgery. The implants used at our clinic have been evaluated by other countries’ registries as those ensuring longest implant life, as compared to products of other manufacturers. Read more here.
13 patients' case studies
Direct flights to Lithuania





What is a total knee replacement?
Knee replacement surgery, also known as arthroplasty, is generally regarded as an effective treatment for end-stage knee arthritis. It results in an improved knee function and significantly relieves severe pain caused by degenerative joint diseases. All knee replacement procedures are generally divided into 2 major groups, depending on whether the knee is replaced totally or partially. When trying to better understand the mechanism behind total knee arthroplasty, knowing the anatomic complexity of a knee comes in handy. A knee joint is often compared to a hinge which allows to flex, extend and limitedly rotate the lower leg. Structurally it resembles three separate joints: slightly rounded end of the thigh bone forms 2 separate articulations with a slightly hollow end of the shinbone which has a mobile kneecap on top. The most common indication for total knee replacement is severe osteoarthritis that affects all surfaces of these synergic joints and causes pain which is unresponsive to medical management.
- During the procedure, the patella is laterally subluxed and the knee is exposed in flexion.
- The affected joint tissue is surgically removed and replaced by a knee prosthesis which consists of three separate components.
- The end of a thigh bone is replaced with a femoral component made out of metal plate which corresponds to the natural shape of the bone.
- The tibial component, which consists of a metal tray covered with a layer of plastic that moves against the surface of the femoral segment, replaces the top surface of the lower leg bone.
- Patellar component covers the back part of the kneecap and is made out of plastic for it to glide over the front of the knee. Due to this reason the patients are advised not to kneel on the operated knee as the plastic covering of the patella may resurface.
These significant structural changes are directly responsible for the main complaint after knee replacement surgery, which is stiffness and a lingering sensation of a foreign body placed inside the joint. All in all, a total knee replacement is one of the most successful examples of innovative surgery and has resulted in substantial quality-of-life gains for people with severe joint problems.
Exclusive to our patients - long-standing X-rays
FAQ about knee replacement with our surgeon
More FAQ videos from our surgeon:
Watch full list of interview sessions on our Youtube channel.
What is a partial knee replacement?
In comparison to a total knee arthroplasty, partial knee replacement may be defined as a less invasive surgical approach for patients with only moderate knee joint diseases. A great majority of degenerative joint diseases primarily affect the medial compartment of the knee joint. This is because a fibrous cartilage between the surfaces of the medial tibiofemoral articulation, also known as a medial meniscus, is relatively thinner and experience greater pressure while walking etc. The damaged component of the knee is replaced using the same method as in the total knee arthroplasty but without affecting the healthy parts of the joint. However, as flawless as partial knee replacement may sound, its biggest potential drawback is incomplete pain relief. The success of the surgery depends entirely on choosing the right candidate and carefully evaluating the extent of disease.
Preparation for surgery
Careful preparation for knee replacement surgery is an important part of the procedure itself as it determines the success of the surgery and the quality of post-op recovery. Here are the main recommendations to be followed:
Practice active lifestyle. Committing to some form of regular exercise may greatly facilitate the recovery. Activities such as swimming or cycling are excellent for maintaining muscle function and range of motion. If the joints are painful and rigid the patient should stay minimally active by only taking short walks several times a day.
It is highly advised to quit smoking and consuming alcohol at least 2 weeks before the procedure as it may impair and delay bone healing.
It is important to stay as healthy as possible before the operation. Following a balanced diet and staying hydrated will strengthen the body, and this will help for a speedy and smooth recovery. The patients with a BMI higher than 25 may be also advised to lose some weight. However, it is important to be well nourished before the procedure therefore a very low-calorie diet just weeks before the surgery is not recommended.
Medications such as nonsteroidal anti-inflammatory drugs, blood thinners and aspirin should be avoided as they may cause bleeding during the procedure.
Consult an operating doctor about your allergies, previous surgeries, food supplements etc. If you have any pre-existing conditions that require daily usage of drugs, make sure to inform the doctor beforehand.
Follow your specific pre-operative instructions as they may vary depending on your medical history. If the instructions are not followed the surgery may be cancelled or postponed.
Is there an age or BMI limit for the surgery?
Increased body weight would, intuitively, be expected to lead to a poorer outcome after joint replacement as the knees are directly strained by overweight. A significant positive correlation has been observed between the wear damage seen on the components of knee prosthesis and the BMI of the postoperative patients. However, some recently published studies have proven that the perioperative complication rate in patients with BMI over 40 wasn’t dramatically higher than the rate in patients with lower BMIs. Moreover, it is now known that obese patients have relatively good pain relief and positive functional outcomes after the surgery. Therefore, a simple answer to the question about BMI limit is negative. Looking from a medical point of view, obesity is associated with many other comorbidities that affect one’s everyday life and well-being. That is why overweight should not be tolerated, and if a patient is able to lose weight they most definitely should do that.
The age limit for knee replacement patients is also of a debatable significance. Although the older patients require a relatively longer hospitalization time and have higher complication rates, the improvements in their quality of life are very similar to those of younger patients.
Hospitalisation and what to expect during the first days after surgery
After the surgery a patient is expected to stay in the clinic for 2 to 3 days. If a patient underwent general anesthesia, it is absolutely normal to experience some mild side effects on the first day after the procedure. On the following day a postoperative patient is encouraged to start moving and walking with a walker or crutches. In the beginning, it requires a lot of will and effort to start walking again, but it will pay off in the form of faster recovery. Upon discharge from the hospital, a patient should be able to take short walks, bend one’s knee up to 90 degrees and climb up and down a few steps with some extra help.
The importance of physiotherapy
It could be said that half of the success of a knee replacement surgery depends on the post-op physical therapy. Physiotherapy exercise routine may be either home-based or monitored by the health professionals in rehabilitation facilities. Studies have shown that light to moderate regular exercises show short-term improvements in patients’ physical function, whereas more intensive ones have positive long-term outcomes. In order for a certain therapeutic approach to give good results the right combination of physiotherapy methods should be selected for each patient individually.
The risk of flying and how to avoid it
As surprising as it may seem, air travel is directly associated with the risk of deep vein thrombosis (DVT) in post-operative patients. It is because prolonged periods of inactivity and space limitations slow down the blood circulation, and the major veins of the knees are compressed creating a potential site for clot formation. Low cabin pressure at high elevations also contributes to making blood thicker. Therefore, the candidates for knee replacement surgery are advised to avoid flying for up to 6 weeks before and after the procedure. If it is necessary for a patient to take a flight one may still do that but some extra precautionary steps should be taken:
- It is usually advised to flex legs frequently during the flight and drink mineral water in order to stay properly hydrated.
- For the patients with a higher risk of thrombosis compression stockings are recommended as they constrict the diameter of veins and increase the blood flow.
- In some cases, blood thinning medications or antiplatelet drugs may be prescribed.
Physical activity after the surgery
The positive effects of physical activity are particularly important for patients undergoing knee replacement, as osteoarthritis predisposes them to metabolic and functional decline. Light physical activity such as walking, climbing the stairs, jogging etc. is an attractive and convenient form of exercise as it can be self-managed and performed on a daily basis with low cost and minimal equipment. In addition to that, there are several types of exercises which target specific muscle groups of the lower body and may be performed every day:
Exercising muscles of the thigh improves knee flexion. This may be achieved by light stretches of hamstrings.
Muscles in the front of the thigh are responsible for knee extension. In order to strengthen them any light tension creating exercises, such as half squats done while holding on to a handrail or straightening the leg while sitting on a chair etc. are advised
In the early post-operative period there is a great variety of light exercises that should be performed while lying down. This includes bending the knees by sliding the heel towards the buttocks, repeatedly adducting the operated leg etc.
In order to choose the right form of exercise which would result beneficial, one should always consult a physiotherapist.
Wound care and staple removal
After the knee is totally or partially replaced, the midline incision across the front of a knee is closed and tightened up with staples or stitches. In order to prevent the wound from getting infected, a waterproof dressing is applied. It is highly recommended to keep the dressing for up to 7 days after the procedure unless it moves out of place or becomes fully saturated. If so, it should be changed by a qualified nurse, if possible, or a patient may do it by themselves.
When it comes to showering, it is allowed as long as the dressing is kept as dry as possible, for it may fall off if the skin becomes too moist.
The stitches or staples are usually removed in 10 to 21 days after the surgery. If during the postoperative period a leakage, bruise or swelling is observed and the incision site becomes painful, you should consult a doctor immediately as the wound might get infected.
Driving after a surgery
The candidates for knee replacement are often hesitant about the surgery as there is a common misconception that driving is prohibited once the surgery is performed. In fact, the postoperative patients may already resume driving 4 weeks post-op or when they feel comfortable and confident about the flexibility of the knee.
Sports after knee replacement
Based on a general opinion among the medical society low-impact sports, such as hiking, swimming, running, and cycling etc. after knee replacement are most certainly welcome and encouraged. However, strenuous activities that put a lot of pressure on the knees are a topic of discussion. It is observed that the patients who played sports before their surgery are more likely to return to sports because of their willingness and motivation. All in all, due to the improvements in surgical technique and the growing knowledge about post-operative management of knee prosthesis, knee replacement surgery has even less impact on the activity level of post-operative patients.
Send us your enquiry