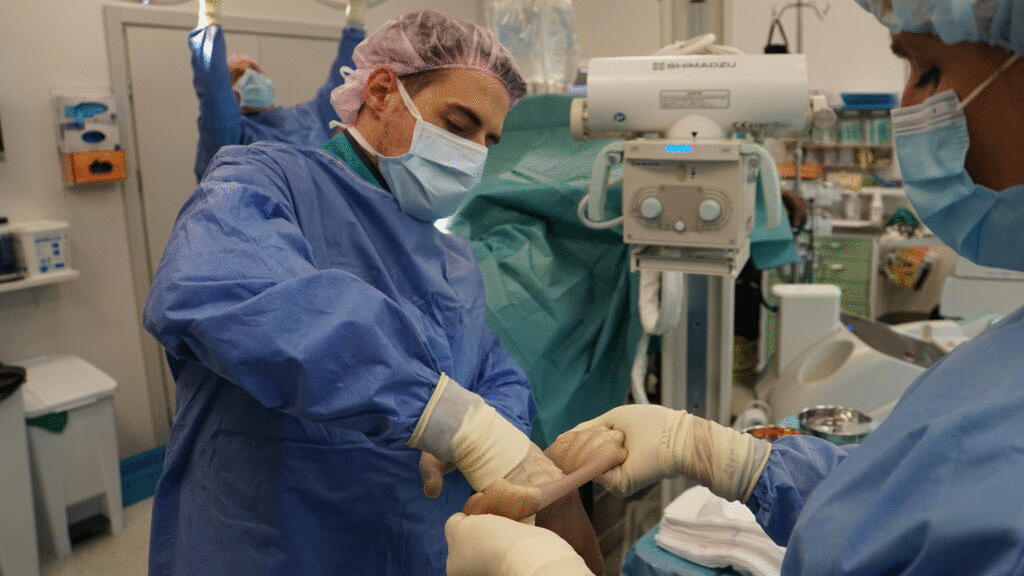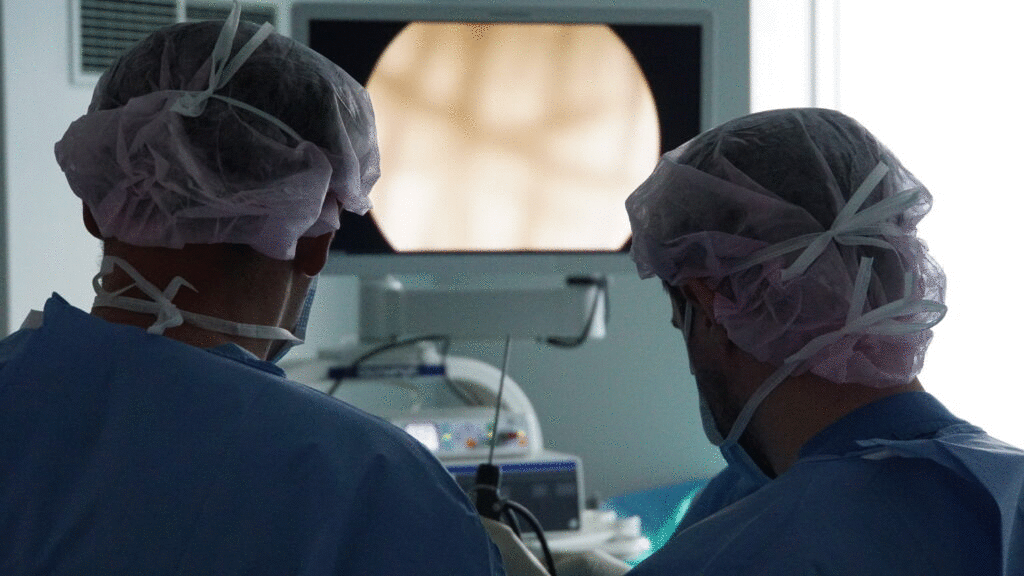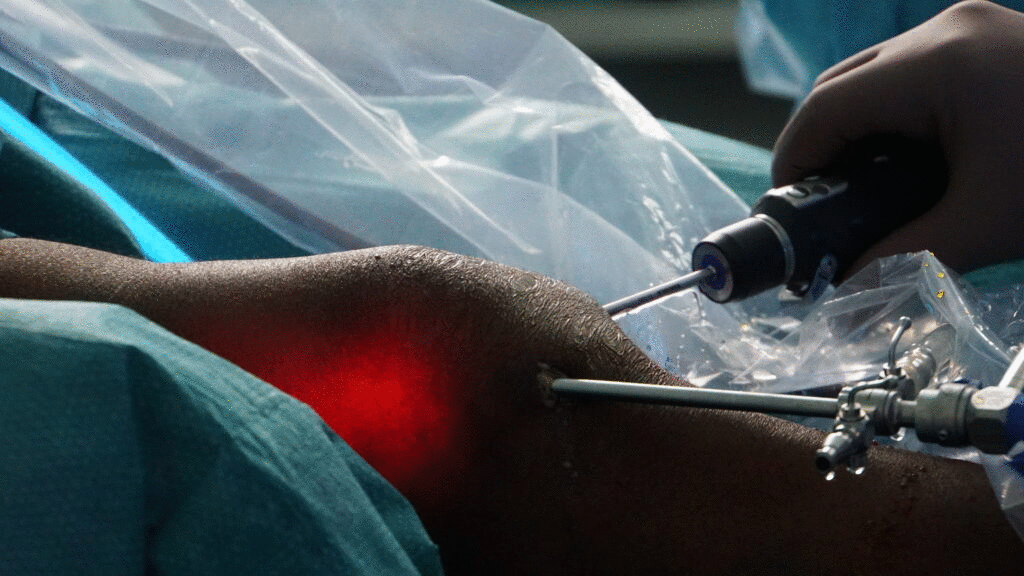
Femoral Osteotomy
We are one of the leading orthopaedic surgery clinics for medical tourists in the European Union. We are proud of the fact that over 90 % of our patients come from the UK, Ireland, Norway, Sweden, the United States, Canada and other countries.
Reviews & Facebook group
Our patients and clinic in the media
Prices
- femoral osteotomy – from 4.300 £
- high tibial osteotomy (1 leg) – 4.130 £
- knee replacement – 6.340 £
- hallux valgus – 1.400 £
- long standing X-ray performed in 1 day – FREE
- accommodation with medical care – from 62 £ per night
- consultation with the surgeon
- necessary health tests
- surgery
- implant
- anaesthesia
- hospitalisation
- 24/7 personal assistance during your stay
- transfers to / from the airport, hotel and clinic
- all documents translated to English
Get your surgery for free by claiming a refund from your local health board. The clinic helps patients with the documents needed to claim a refund after following the EU directive route for medical treatment abroad. It applies to patients who are insured under the systems of one of the EU countries and may not get the surgery due to long waiting times.
- femoral osteotomy – from 5.160 €
- high tibial osteotomy (1 leg) – 4.660 €
- knee replacement – 7.600 €
- hallux Valgus – 1.710 €
- long standing X-ray performed in 1 day – FREE
- accommodation with medical care – from 74 € per night
- consultation with the surgeon
- necessary health tests
- surgery
- implant
- anaesthesia
- hospitalisation
- 24/7 personal assistance during your stay
- transfers to / from the airport, hotel and clinic
- all documents translated in English
Get your surgery for free by claiming a refund from your local health board. The clinic helps patients with the documents needed to claim a refund after following the EU directive route for medical treatment abroad. It applies to patients who are insured under the systems of one of the EU countries and may not get the surgery due to long waiting times.
Femoral Osteotomy case analysis
Patient stories
Clinic videos
Nordorthopaedics Center Of Excellence

Refund for EU patients
Get your surgery for free by claiming a refund from your local health board. The clinic helps patients with the documents needed to claim a refund after following the EU directive route for medical treatment abroad. It applies to patients who are insured under the systems of one of the EU countries and may not get the surgery due to long waiting times. On average our patients from the EU countries get fully refunded by their local health board in 5 months after their surgeries.
Rehabilitation package
One of the most important factors for a quick and full recovery after surgery is proper rehabilitation. Rehabilitation helps recover after surgery as well as prevents formation of blood clots and helps avoid most of the postoperative complications and side effects. Outpatient rehabilitation in Kaunas with a physiotherapist.
The rehabilitation clinic is equipped with modern facilities. Individual rehabilitation programs are prepared by a kinesiologist with over 20 years of experience, Prof. Laimonas Siupsinskas. This type of rehabilitation is best suited for people who are physically active, athletes and those wishing to return to sports as soon as possible.
Rehabilitation in Kaunas – € 120 / £ 100 for one 1 h physiotherapy session per day.
- personalized rehabilitation course;
- specialist who is also a physiotherapist for Lithuanian Men’s National Basketball Team;
- all required medication;
- transportation to/from the rehabilitation clinic;
- read more about outpatient rehabilitation in Kaunas.
Our clinic
Self-catered accommodation with medical care
11 reasons that make us the most popular orthopaedic clinic abroad
One of the most important factors for a quick and full recovery after surgery is proper rehabilitation. Usually, clinics are not able to offer this due to costs savings. Our patients can choose between two inpatient and outpatient options: rehabilitation with a physiotherapist of the Lithuanian national basketball team, prof. L. Siupsinskas or rehabilitation at a medical SPA.
Our team of 5 orthopaedic surgeons has 10-20 years of experience in the field in total performing over 1.000 different orthopaedic surgeries per year. Moreover, our surgeons are members of various prestigious surgical societies both Lithuanian and international. Our leading joint replacement surgeon S. Tarasevicius is an author of 150 scientific publications in different medical journals, who has performed more than 3.500 joint replacement surgeries during 15+ years of his professional experience.
We are one of the leading orthopaedic surgery clinics for medical tourists in the European Union. We are proud of the fact that over 90 % of our patients come from the UK, Ireland, Norway, Sweden, the United States, Canada and other countries.
One of the world’s leading medical technology companies and orthopaedic implant manufacturers, Smith & Nephew, have chosen Nordorthopaedics as Center of Excellence in the Baltic States.
We are trusted by our patients and we appreciate all the reviews and feedback collected over the years. Find more than 150 testimonials here or on Google.
Already more than 4.000 of our former, current and future patients joined our online community with the aim to build a space for opinions and mutual support. Members are welcome to share experiences about their visit to the clinic and to discuss all surgery-related matters. No other orthopaedic clinic can offer such group support.
Being a true member of the International Society of Arthroplasty Registries, Lithuania is one of the leaders in low joint replacement revision rates, as only 9% of surgeries in Lithuania require revision in 10 years after surgery. Moreover, with the implants used at our clinic, only 2-3% of surgeries require revision in 10 years after surgery, while revision rates in some other Western countries, for example, USA, is as high as 17% in 10 years after surgery. The implants used at our clinic have been evaluated by other countries’ registries as those ensuring longest implant life, as compared to products of other manufacturers. Moreover, thanks to our active participation in collecting data for the registries, the surgical technique used at our clinic ensures best surgical outcomes.
Our clinic is seen on different media mentions like: BBC News, BBC Radio, The Telegraph, MailOnline, Winnipeg Free Press, CTV News, CBC, RTE Radio, itv.
Our clinic works according to the highest standards set by the European Union. This helps to guarantee the quality of medical services. We care about the safety, comfort and successful results of our patients from all over the world.
The clinic helps patients with the documents needed to claim a refund after following the EU directive route for medical treatment abroad. It applies to patients who are insured under the systems of one of the EU countries and may not get the surgery due to long waiting times.
We provide customer service in 9 foreign languages including English, Swedish, Norwegian, Danish, Italian, Spanish, French, Russian, Polish. Everyone in our clinic speaks English, including nurses, assistants and the surgeon.
Athletes treated at Nordorthopaedics
Official clinic of Lithuania national football teams

Highest quality implants
Our clinic uses implants based on their performance in international registries.
Being a true member of the International Society of Arthroplasty Registries, Lithuania is one of the leaders in low joint replacement revision rates, as only 9% of surgeries in Lithuania require revision in 10 years after surgery. Moreover, with the implants used at our clinic, only 2-3% of surgeries require revision in 10 years after surgery, while revision rates in some other Western countries, for example, USA, is as high as 17% in 10 years after surgery. The implants used at our clinic have been evaluated by other countries’ registries as those ensuring longest implant life, as compared to products of other manufacturers. Read more here.
13 patients' case studies
What is femoral osteotomy?
Femoral osteotomy, also known as a knock knees surgery, is a surgery done on the thigh bone above the knee cap. It is most often performed for patients with ostheoarthritis or a valgus knee deformity (also called a “knock-knee” deformity). The surgery realigns the upper and lower leg bones, making the weight-bearing axis pass through the center of the knee. Femoral osteotomy ensures equal weight distribution, addresses gait abnormalities, relieves symptoms of arthritis, and slows the development of degenerative joint disease.
Who is a good femoral osteotomy candidate? What conditions can femoral osteotomy treat?
Femoral osteotomy is generally recommended for young (<55 years old) and active patients. The main two femoral osteotomy indications are:
- Valgus knee, also known as a knock knee deformity. Open wedge technique is a precise technique that accurately corrects the knee alignment, shifting mechanical axis to the center of the knee joint.
- Arthritis on the outside of the knee. Straightening out the femur realigns the mechanical axis and unloads weight from the damaged cartilage.
What are femoral osteotomy risks?
All surgeries come with a certain level of risk. Even though femoral osteotomy has been performed for decades and the benefits far outweigh the risks, complications can occur in rare instances. Some of the possible complications include post-operative bleeding, wound infection, blood clots, neurovascular damage, and other.
How to prepare for femoral osteotomy?
During an initial consultation, an orthopaedic surgeon takes a patient’s health history, discusses the expectations, and orders imaging tests, like an X-ray and MRI scan. A complete knee examination is performed to assess joint tenderness, meniscal pathology, and ligamentous instability. The patient should be prepared to state any allergies and bring a list of all the medications, including all prescription and over-the-counter drugs as some of them can cause bleeding problems during surgery.
Two weeks before surgery, patients must refrain from smoking as doing so significantly increases clotting risk.
Patients are advised to follow a healthy diet and consume enough zinc, iron, and vitamins A, D, and C.
Patients are also recommended to purchase crutches, stock up with easy-to-cook meals, and arrange help at home. It is a good idea to temporarily move the bedroom downstairs or rearrange the furniture to make more space for moving with assistive devices.
On the day of surgery, patients should not eat at least 6 hours and not drink at least 2 hours before surgery. We recommend patients leave any valuable items at home and arrive wearing comfortable loose-fitting clothes.
What happens during femoral osteotomy?
The goal of femoral osteotomy is to re-create a correct alignment between an upper thigh bone (femur) and lower leg bones (tibia and fibula). Surgery is performed under general anaesthesia and takes approximately 2 hours to complete. There are two main surgical techniques to realign the knees.
In open wedge osteotomy, a surgeon makes a 4 cm incision on the outside of the knee and dissects the muscles to expose the femur bone. Then, he separates the two sides of the femur with special retractors to form a wedge shape. The created space is filled with synthetic bone graft to secure the correct mechanical axis. Lastly, the surgeon places a drain inside the incision to help remove fluids and fasten recovery.
A medial closing wedge osteotomy requires a 10 cm longitudinal incision on the inner side of the knee joint. A surgeon dissects the muscles, exposes the femur, and cuts out a wedge of the femur bone. After removal of the bone wedge, the fracture gap is brought together and secured with a titanium plate. Once the desired knee alignment is obtained, a surgeon inserts a drain, closes the incision, and places the knee in a surgical dressing.
What happens after femoral osteotomy?
- Following surgery, the operated knee is placed in a large bandage and a knee brace.
- Patients begin moving the leg as soon as the drain is removed, usually the next day post-op.
- Recovery involves lots of rest and the leg should be kept elevated as much as possible. Patients are allowed to bear weight on the operated leg as far as pain allows.
- Pain relievers, like naproxen, are prescribed to control post-op discomfort.
- Patients are usually discharged after 2 to 3 days post-op.
- While at home, the bandage should be changed every 3-5 days. The post-operative recovery also involves regular exercising to improve muscle tonus and prompt recovery.
How long does it take to recover after femoral osteotomy?
During the first 6 weeks post-op, patients take blood-thinning drugs (aspirin), walk with crutches, and exercise regularly to improve range of motion. In two weeks, patients see their doctor to take out the staples. At the end of 6 weeks, patients come in for a follow-up X-ray scan.
After another 6 weeks, most patients can return to work and transition to cane or crutches. Exercises include gentle stretching, strengthening, and walking. Patients should expect to come in for a second X-ray scan to evaluate how well the bones are healing. A return to driving is possible at 6-10 weeks post-operatively.
Most patients can return to leisure sports, like walking, hiking, cycling, swimming, and tennis. It may be 6 to 9 months until resuming high-impact activities.
Send us your enquiry