Knee Arthroscopy Abroad: Lithuania
We are one of the leading orthopaedic surgery clinics for medical tourists in the European Union. We are proud of the fact that over 90 % of our patients come from the UK, Ireland, Norway, Sweden, the United States, Canada and other countries.
Reviews & Facebook group
Our patients and clinic in the media
Prices
- knee arthoscopy – 2.000 £ | or 750 £ with S2 funding*
- knee replacement – from 6.340 £
- MRI performed in 1 day – from 155 £
- 2 online prehab consultations (upon request) – 86 £
- rehabilitation after surgery – from 100 £ per day
*Your surgery can be partly funded via the S2 funding route (read more in the next tab)
- accommodation with medical care – from 62 £ per night
The S2 route may entitle you to NHS funding for planned state healthcare treatment in Lithuania. You can save up to 60% for the knee arthroscopy surgery. Contact our customer service for more information:
- Knee arthroscopy
- 2.000 £ without S2 funding
- 750 £ with S2 funding
- consultation with the surgeon
- necessary health tests
- surgery
- anaesthesia
- hospitalisation
- 24/7 personal assistance during your stay
- transfers to / from the airport, hotel and clinic
- all documents translated to English
Get your surgery for free by claiming a refund from your local health board. The clinic helps patients with the documents needed to claim a refund after following the EU directive route for medical treatment abroad. It applies to patients who are insured under the systems of one of the EU countries and may not get the surgery due to long waiting times.
- knee arthroscopy – 2.400 € | or 900 € with S2 funding*
- knee replacement – from 7.600 €
- MRI performed in 1 day – from 180 €
- 2 online prehab consultations (upon request) – 100 €
- rehabilitation after surgery – from 120 € per day
*Your surgery can be partly funded via the S2 funding route (read more in the next tab)
- accommodation with medical care – from 74 € per night
The S2 route may entitle you to NHS funding for planned state healthcare treatment in Lithuania. You can save up to 60% for the knee arthroscopy surgery. Contact our customer service for more information:
- Knee arthroscopy
- 2.400 € without S2 funding
- 900 € with S2 funding
- consultation with the surgeon
- necessary health tests
- surgery
- anaesthesia
- hospitalisation
- 24/7 personal assistance during your stay
- transfers to / from the airport, hotel and clinic
- all documents translated to English
Get your surgery for free by claiming a refund from your local health board. The clinic helps patients with the documents needed to claim a refund after following the EU directive route for medical treatment abroad. It applies to patients who are insured under the systems of one of the EU countries and may not get the surgery due to long waiting times.
Meniscus repair case analysis
Patient stories
Clinic videos
Nordorthopaedics Center Of Excellence

Our surgeon Valdemar Loiba

- More than 15 years of working experience
- Performs 400+ arthroscopies a year.
- Author of 6 international oral presentations
- Read more
Refund for EU patients
Get your surgery for free by claiming a refund from your local health board. The clinic helps patients with the documents needed to claim a refund after following the EU directive route for medical treatment abroad. It applies to patients who are insured under the systems of one of the EU countries and may not get the surgery due to long waiting times. On average our patients from the EU countries get fully refunded by their local health board in 5 months after their surgeries.
Rehabilitation packages
One of the most important factors for a quick and full recovery after surgery is proper rehabilitation. Rehabilitation helps recover after surgery as well as prevents formation of blood clots and helps avoid most of the postoperative complications and side effects. We offer two different rehabilitation packages:
Outpatient rehabilitation in Kaunas with a physiotherapist. The rehabilitation clinic is equipped with modern facilities. Individual rehabilitation programs are prepared by a kinesiologist with over 20 years of experience, Prof. Laimonas Siupsinskas. This type of rehabilitation is best suited for people who are physically active, athletes and those wishing to return to sports as soon as possible.
Rehabilitation in Kaunas – € 120 / £ 100 for one 1 h physiotherapy session per day.
- personalized rehabilitation course;
- specialist who is also a physiotherapist for Lithuanian Men’s National Basketball Team;
- all required medication;
- transportation to/from the rehabilitation clinic;
- read more about outpatient rehabilitation in Kaunas.
Inpatient rehabilitation at SPA resort in Druskininkai. It is equipped with modern facilities. The professionals there have years of experience working with people after various surgeries and injuries.
Rehabilitation at SPA resort in Druskininkai – from € 220 / £ 183 per day
- personalized rehabilitation course;
- room with TV and private bathroom;
- three meals a day;
- all medication needed;
- transportation to/from the rehabilitation centre;
- read more about inpatient rehabilitation in Druskininkai.
Our clinic
Self-catered accommodation with medical care
11 reasons that make us the most popular orthopaedic clinic abroad
One of the most important factors for a quick and full recovery after surgery is proper rehabilitation. Usually, clinics are not able to offer this due to costs savings. Our patients can choose between two inpatient and outpatient options: rehabilitation with a physiotherapist of the Lithuanian national basketball team, prof. L. Siupsinskas or rehabilitation at a medical SPA.
Our team of 5 orthopaedic surgeons has 10-20 years of experience in the field in total performing over 1.000 different orthopaedic surgeries per year. Moreover, our surgeons are members of various prestigious surgical societies both Lithuanian and international. Our leading joint replacement surgeon S. Tarasevicius is an author of 150 scientific publications in different medical journals, who has performed more than 3.500 joint replacement surgeries during 15+ years of his professional experience.
We are one of the leading orthopaedic surgery clinics for medical tourists in the European Union. We are proud of the fact that over 90 % of our patients come from the UK, Ireland, Norway, Sweden, the United States, Canada and other countries.
One of the world’s leading medical technology companies and orthopaedic implant manufacturers, Smith & Nephew, have chosen Nordorthopaedics as Center of Excellence in the Baltic States.
We are trusted by our patients and we appreciate all the reviews and feedback collected over the years. Find more than 150 testimonials here or on Google.
Already more than 4.000 of our former, current and future patients joined our online community with the aim to build a space for opinions and mutual support. Members are welcome to share experiences about their visit to the clinic and to discuss all surgery-related matters. No other orthopaedic clinic can offer such group support.
Being a true member of the International Society of Arthroplasty Registries, Lithuania is one of the leaders in low joint replacement revision rates, as only 9% of surgeries in Lithuania require revision in 10 years after surgery. Moreover, with the implants used at our clinic, only 2-3% of surgeries require revision in 10 years after surgery, while revision rates in some other Western countries, for example, USA, is as high as 17% in 10 years after surgery. The implants used at our clinic have been evaluated by other countries’ registries as those ensuring longest implant life, as compared to products of other manufacturers. Moreover, thanks to our active participation in collecting data for the registries, the surgical technique used at our clinic ensures best surgical outcomes.
Our clinic is seen on different media mentions like: BBC News, BBC Radio, The Telegraph, MailOnline, Winnipeg Free Press, CTV News, CBC, RTE Radio, itv.
Our clinic works according to the highest standards set by the European Union. This helps to guarantee the quality of medical services. We care about the safety, comfort and successful results of our patients from all over the world.
The clinic helps patients with the documents needed to claim a refund after following the EU directive route for medical treatment abroad. It applies to patients who are insured under the systems of one of the EU countries and may not get the surgery due to long waiting times.
We provide customer service in 9 foreign languages including English, Swedish, Norwegian, Danish, Italian, Spanish, French, Russian, Polish. Everyone in our clinic speaks English, including nurses, assistants and the surgeon.
Athletes treated at Nordorthopaedics
Official clinic of Lithuania national football teams

Highest quality implants
Our clinic uses implants based on their performance in international registries.
Being a true member of the International Society of Arthroplasty Registries, Lithuania is one of the leaders in low joint replacement revision rates, as only 9% of surgeries in Lithuania require revision in 10 years after surgery. Moreover, with the implants used at our clinic, only 2-3% of surgeries require revision in 10 years after surgery, while revision rates in some other Western countries, for example, USA, is as high as 17% in 10 years after surgery. The implants used at our clinic have been evaluated by other countries’ registries as those ensuring longest implant life, as compared to products of other manufacturers. Read more here.
13 patients' case studies
Direct flights to Lithuania





What is knee arthroscopy and why is it performed?
Knee arthroscopy is a surgical technique that allows a surgeon to view the inside of the knee and treat the damaged ligaments of the knee joint.
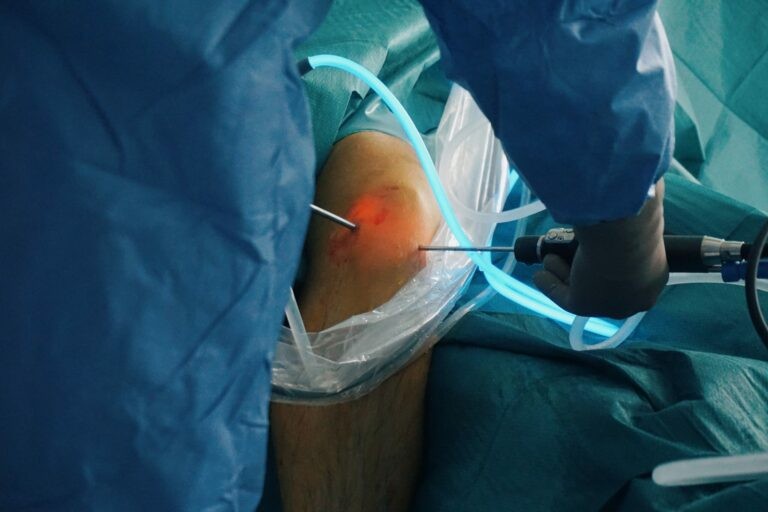
During knee arthroscopy the surgeon makes a few small incisions in the knee and injects saline. Saline is a salty aqueous solution which expands the knee, and therefore, provides the surgeon with a clear sight of the joint.
A tiny camera, which is called an arthroscope, is inserted into the knee making it possible for the surgeon to view inside of the joint and repair the damaged ligaments with a great precision.
Knee arthroscopy is a procedure of choice for diagnosing knee problems and then treating them.
The arthroscopic view provides detailed imaging of the knee which helps to diagnose the problem, confirm a source of pain, or treat the damaged ligaments. Doctors often use arthroscopy when other imaging techniques (e.g. X-rays or MRI) have failed to provide enough information about the injury. Usually knee arthroscopy is used for diagnosing torn meniscus and patellar tracking issues.
Types of meniscus tears
Menisci are located between tibia and femur bones. These ligaments are composed of cartilaginous tissue and may resemble rubbery cushions which function as ‘shock absorbers’. Menisci highly contribute to keeping the knee stable and protecting the bones from grinding into each other when moving.
Knee injuries mostly include various manifestations of the meniscal tears. Menisci are often torn because of traumatic events, injury, or degeneration, and anyone at any age can have their meniscus damaged. The injury may be caused by sudden twisting, rotating or squatting movements. Surgeons usually recommend arthroscopic knee surgery for the injuries that remain symptomatic. If a meniscus tear remains untreated, the risk of developing osteoarthritis later in life increases significantly. The choice of surgical method depends on the type of meniscus tear.
- An incomplete tear usually does not require surgical treatment since this type of injury is relatively stable. Sometimes it may heal on its own, however, consulting a doctor and choosing a treatment plan is crucial for a successful recovery.
- A radial tear has little to no capacity to heal since the tear is usually located in the central part of the meniscus where there is no blood supply. Hence, the damaged portion has to be fully removed during surgery.
- A horizontal tear does not require removing a part of the meniscus and can rather be treated by sewing the torn parts together.
- A flap tear is an uncommon pattern of a meniscus injury. It may prevent the knee from bending smoothly, cause pain and instability. Fortunately, a flap tear can be simply treated without a need to remove a large portion of the meniscus.
- A bucket-handle is a horizontal tear along meniscus. The torn portion of the meniscus usually cause the knee to become stuck, and therefore, limits normal range of motion. Bucket-handle tears require immediate surgical treatment to restore a usual bending of the knee.
The symptoms and diagnosis of a meniscus tear
A meniscal tear is usually a result of a trauma or degenerative processes, and can be quite painful and debilitating. When the meniscus is damaged one is likely to hear a ‘pop’ sound and feel a ‘tearing’ sensation in the knee. Many people choose to continue walking even when their knee is injured. Unfortunately, the knee slowly swells and after approximately 6-12 hours becomes stiff and painful. A meniscal tear might also result in a free body, which can obstruct full knee flexion leading to a locked flexion.
In this case the patient might not be able to move the knee to its full range of motion. A meniscus tear can be diagnosed if there is tenderness within the joint, the joint is significantly effused, or there is a limited range of motion. There are specific tests which help to determine if the meniscus is torn, however, meniscal tears are best diagnosed through MRI scanning.
Preparing for arthroscopic knee surgery
In order to experience a stress-free recovery it is necessary to prepare for an upcoming surgery in advance. During a consultation with a surgeon, a patient’s medical history and all the medications in use will be reviewed. The patient is asked about the current health and the previous medical, surgical, and medication history.
The doctor might recommend discontinuing aspirin, ibuprofen, CoQ10, glucosamine chondroitin, flaxseed, vitamin E, fish oil, green tea, chia seeds, primrose oil, and garlic as they all increase the risk of bleeding.
Also, the patient should avoid tobacco and alcohol consumption a month before and after the surgery since these substances disrupt and prolong the healing process.
It is advised to move downstairs for at least a couple of weeks and avoid using the stairs to refrain from putting weight on the operated knee. The patient should prepare a few pillows which will be placed under the operated knee since elevating the leg reduces postoperative swelling and speeds up recovery.
One week before the surgery the patient should undergo all the necessary medical tests. All the aspects of the surgery, such as available strategies and post-operative period, will be discussed during a private consultation. The patient will have to undergo any necessary lab tests, including blood work, urine test, ECG (electrocardiogram), X-rays, or others.
During the surgery a patient is given general anaesthesia. In order to prevent regurgitation during the surgery, the patient cannot eat or drink at least 6 hours before the surgery. It is extremely important that one does not have any bruises, cuts, or pimples on the legs as they highly increase the risk of infection. Patients are recommended to arrive a few hours before the surgery and bring all the medications they might need additionally. Wearing loose and comfortable clothing will make it easier to dress up when leaving the hospital.
Hospitalization and what to expect on the first few days after the surgery
Once the patient has recovered from anaesthesia they will find themselves in a recovery room. The knee will be bandaged and elevated. The patient might feel more or less tired which is common after undergoing anaesthesia. Many patients can be discharged from the hospital as soon as 2 hours post-surgery.
Usually, it is possible to return back to a sitting job after approximately a week and other daily activities may be resumed in 3 weeks. Returning to sports takes more time but most people can come back to high intensity activities in a few months.
After the surgery the knee may ache and swell. Recovery time varies depending on many factors. Most patients remain active after the treatment of a torn meniscus, broken cartilage, or Baker’s cyst, and does not even need to use assistive devices. The patients are recommended to wear a hinged knee brace for 4 weeks post-surgery.
The bandages should be kept dry and clean. Patients will be informed about the first time they can have a shower and how to take care of the wound.
For pain control the doctor may recommend taking anti-inflammatory drugs, such as ibuprofen or paracetamol. It is recommended to have someone to check on the patient for the first 24 hours after the surgery. The patient’s knee should be elevated for the first few days to reduce swelling. It is advised to apply ice compresses which helps to alleviate pain and promote healing.
The patient is not allowed to drive until the doctor agrees on doing so.
A rehabilitation specialist will provide a recovery program which usually includes an exercise routine and may include other muscle-strengthening activities, such as swimming, interferential current therapy (ICF), or electrical muscles stimulation.
Physical therapy; returning to sports
Week 1 to 4
During the first week, the goals are to diminish inflammation and swelling, restore knee extension and flexion (90 º), regain Quad muscle activity, full scar and patellar mobility. Such exercises as ankle pumps, quadriceps and hamstring sets and gluteal sets aid in strengthening the muscles used in knee bending.
Week 4 to 6
This time is dedicated to restoring the active range of motion (AROM) and reestablishing muscle activity. The goal is to move with no painful sensations. Training proprioception is an important part of the recovery too. The patient will do such exercises as heel raises, mini-squats (knees are bent less than 90 º degrees), and may use a stationary bike without resistance.
Week 6 to 12
At this time, the patients are prepared for advanced exercises. A range of motion should be full and pain-free. Patients can now begin to flex the knee beyond 90º. Depending on the individual cases, kinesiotherapist will offer advanced exercises which enhance stability and flexibility of the knee.
Week 12-16
People who are looking to return to professional sports should continue to increase muscle strength, power, and endurance. At this time, sport-specific training can be introduced. However, the patients are still recommended to avoid squatting, pivoting or twisting on the knee. One should continue all exercises and may begin light jogging. Plyometrics and swimming are also highly beneficial in recovery.
Send us your enquiry