Discectomy Abroad: Lithuania
Testimonials









Reviews & Facebook group
As seen on
Our patients in the media
Refund for EU patients
Get your surgery for free by claiming a refund from your local health board. The clinic helps patients with the documents needed to claim a refund after following the EU directive route for medical treatment abroad. It applies to patients who are insured under the systems of one of the EU countries and may not get the surgery due to long waiting times.
Rehabilitation package
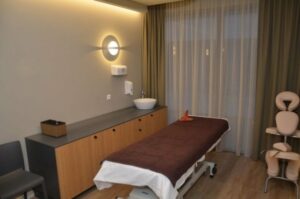
The rehabilitation centre is located at a SPA resort town called Druskininkai. It is equipped with modern facilities. The professionals there have years of experience working with people after various surgeries and injuries.
Rehabilitation in Lithuania – from € 130 / £ 116 per day
- personalized rehabilitation course
- room with TV and private bathroom
- three meals a day
- all medication needed
- transportation to/from the rehabilitation centre
An individual rehabilitation program is prepared for each patient depending on the type of surgery, general patient‘s well-being, health status and other factors.
Our rehabilitation centre
Our clinic
What sets us apart from other clinics?
Our clinic works with highly professional and educated surgeons. They have 10-20 years of experience in the field of orthopaedic surgery. They each perform 500 surgeries per year. Moreover, our surgeons are members of various prestigious surgical societies both Lithuanian and international. Our joint replacement surgeon S. Tarasevicius is an author of 150 scientific publications in different medical journals. Find more information about our surgeons here.
Our clinic works according to the highest standards set by the European Union. This helps to guarantee the quality of medical service.
During your entire stay in Lithuania you will receive personal care as well as transport to and from the clinic, hotel, and airport. You will not have to worry about a thing. You will be assisted from the moment of plane landing in Vilnius or Kaunas airport till your departure.
We have no waiting line so we can schedule your surgery as soon as you are ready to do so.
Everyone in our clinic speaks English, including nurses, assistants and the surgeon.
2-3 hour regular flights operate from all main airports in the UK & Ireland. Lithuania is closer than you thought. You can find the list of direct flights here. Please note that airlines constantly add new flights and new destinations, therefore feel free to contact us if you need help choosing the flight that suits you best.
Lithuania has been a part of the EU and NATO since 2004. Lithuania has one of the fastest growing economies in the whole region and the second fastest internet speed in the world. Lithuanian medical schools have trained many medical professionals who are highly appreciated and employed by many foreign hospitals, among which hospitals in the UK. Our clinic works according to the highest standards set to the medical institutions by the European Union.
Discectomy
Discectomy refers to the surgical removal of the damaged part of a herniated spinal disc. The goal of this surgery is to relieve the pressure on spinal nerves roots that causes pain.
Why is it necessary?
Discectomy is performed in order to relieve the pressure that the herniated disc places on adjacent spinal nerves. Spinal disc herniation is a medical condition in which the outer wall of the disc (annulus fibrosus) becomes weak or it gets torn, thus allowing the inner jelly-like part of the disc (nucleus pulposus) to erupt. In some cases, spinal disc herniation can occur without any symptoms. In other cases altered disc is pressing a spinal nerve and causes pain that can spread from the back to buttocks and legs. The pain limits everyday activities and decreases quality of life. If conservative treatment (rest, physical therapy and medications) does not relieve the pain, surgery may be recommended.
How is discectomy performed?
The goal of discectomy is to decompress spinal nerve root and relieve the pain. Usually, surgeons try to remove only a portion of the disc that is pinching the nerve. There are several types of discectomy such as open discectomy and minimally invasive techniques, including microdiscectomy, endoscopic discectomy and laser discectomy.
Open discectomy. A surgeon approaches the spine through a 3 cm (1 in) long incision in the back. Retractors are placed to hold muscles and skin away from the vertebrae and disc. Once the surgeon reaches the herniated disc, he or she moves the spinal nerve aside with a special retractor. Then the surgeon removes the damaged part of the disc and returns the nerve to its normal position. Finally, the incision is closed and sterile bandage is placed.
Microdiscectomy. This procedure requires a small 1 cm (0.5 in) long incision in the back (usually, through the skin only). The incision is located directly over the herniated disc with the help of a fluoroscope (continuous x-ray image on a monitor). A surgeon places a tube through the incision and starts inserting a series of dilators in order to spread the muscles rather than cut them. The entire surgery is performed through a 2.4 cm (0.9 in) in diameter tube with the assistance of a microscope.
Percutaneous endoscopic discectomy. This is another minimally invasive technique which is very similar to microdiscectomy. The main difference is that in endoscopic discectomy the surgeon uses a surgical endoscope (a device with light and camera) instead of a microscope. The endoscope is inserted through the tube and helps to visualize the spine. The doctor removes a herniated portion of the disc through the same tube.
Percutaneous laser discectomy. The approach to the spine is very similar to other minimally invasive techniques. The difference is that in laser discectomy the damaged part of the herniated disc is not removed. Instead of removal, the jelly-like nucleus pulposus is burnt by the laser.
Possible risks and complications
In general, discectomy is considered as safe procedure with complications rate lower than 1%. These complications include infection, thromboembolic complications, damage to nerves and vessels. Moreover, recurrent disc herniation may occur in 3% to 18% of patients at some point in the future. The only reported complication of laser discectomy is infection of the disc, but it is extremely rare.
Send us your enquiry